9.5 Treating Infection
Antibiotics are used to treat bacterial infections. They either kill bacteria or stop them from reproducing, allowing the body’s natural defenses to eliminate the pathogens. Used properly, antibiotics can save lives. However, growing antibiotic resistance is curbing the effectiveness of these drugs. Taking an antibiotic as directed, even after symptoms disappear, is key to curing an infection and preventing the development of resistant bacteria.
Antibiotics do not work against viral infections such as colds or influenza. Antiviral drugs, which fight infection either by inhibiting a virus’s ability to reproduce or by strengthening the body’s immune response to the infection, are used for some viral infections. There are several different classes of drugs in the antiviral family, and each is used for specific kinds of viral infections.
Antifungal medications are used to treat fungal and yeast infections. Antiparasitic medication is used to treat parasites, and anthelmintic medication is used to treat worm infections.
Antibiotic Stewardship
Microorganisms can quickly develop new features that make them resistant to the drugs that were once able to kill them. People infected with antibiotic-resistant organisms are more likely to have longer, more expensive hospital stays and may be more likely to die as a result of an infection.[1]
Misuse of antimicrobials is one of the world’s most pressing public health problems because of these consequences. Many factors contribute to resistance, including overprescription of antibiotics for nonbacterial infections, use of inappropriate antibiotics for the infectious microorganism, and lack of completion of prescribed antibiotic therapy. Some infections, such as Methicillin-resistant Staphylococcus aureus (MRSA) and Vancomycin-resistant Enterococci (VRE), are becoming increasingly hard to treat and some microorganisms cannot be effectively destroyed by any known antibiotic.[2]
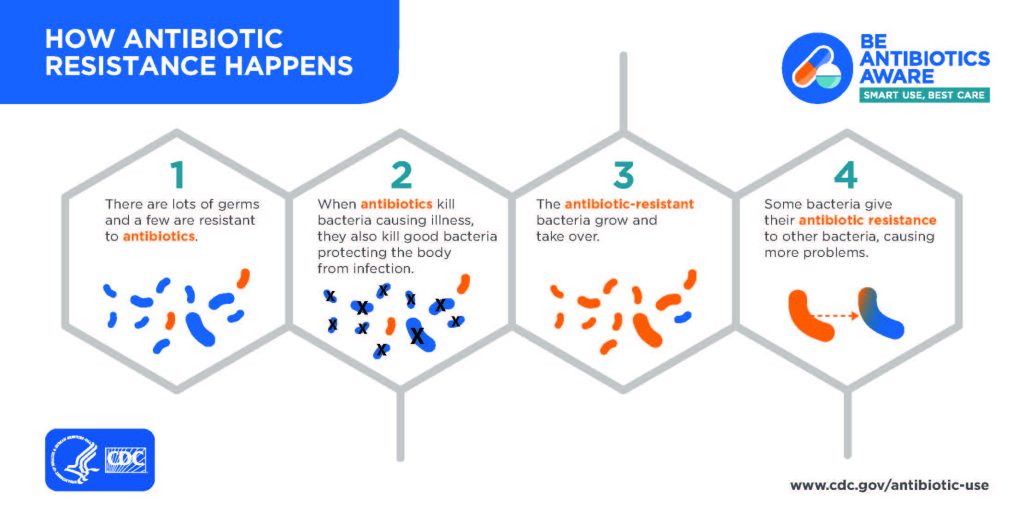
Antimicrobial stewardship is a coordinated program that promotes the appropriate use of antimicrobials (including antibiotics), improves patient outcomes, reduces microbial resistance, and decreases the spread of infections caused by multidrug-resistant organisms. The Centers for Disease Control (CDC) has developed core elements for antibiotic stewardship to serve as a guide to improve antibiotic use for improved patient safety and outcomes.[3] See Figure 9.15[4] for an image from the CDC explaining antibiotic resistance.
The nurse plays an important role in antimicrobial stewardship through patient education. For example, many patients expect to receive an antibiotic when they seek treatment for an illness or symptom. However, because antibiotics are only effective in treating bacteria, the patient should be educated regarding effective treatment for the type of pathogen causing their symptoms. If an antibiotic is prescribed, patients should be advised to complete the entire course of therapy or contact their provider if they are unable to do so. For example, patients often feel better after a few days of treatment and decide not to take the remaining medication, or they may experience side effects from the antibiotic (such as nausea and diarrhea) and stop taking the medication. All of these behaviors can lead to antibiotic resistance and should be addressed when providing patient education regarding prescribed antibiotic therapy.
- Centers for Disease Control and Prevention. (2019, August 15). Core elements of antibiotic stewardship. https://www.cdc.gov/antibiotic-use/core-elements/index.html ↵
- Centers for Disease Control and Prevention. (2019, August 15). Core elements of antibiotic stewardship. https://www.cdc.gov/antibiotic-use/core-elements/index.html ↵
- Centers for Disease Control and Prevention. (2019, August 15). Core elements of antibiotic stewardship. https://www.cdc.gov/antibiotic-use/core-elements/index.html ↵
- “HowAntibioticResistanceHappens.jpg” by CDC is licensed under CC0. Access for free at https://www.cdc.gov/antibiotic-use/community/materials-references/graphics.html. ↵

